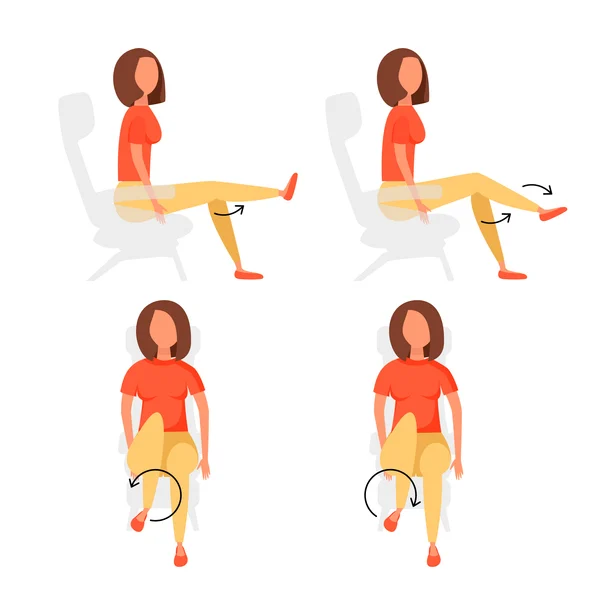
Incorporating knee exercises into your daily routine will improve the strength of your knees.
Knee pain can prevent you from enjoying your favorite activities. The knees allow us to perform daily activities such as climbing, walking, and running. They also bear 40% of our body weight when standing and 150% when we are walking. For your knees to remain healthy and perform optimally, a physical therapist may recommend knee strengthening exercises to prevent injury and pain caused by aging, stress, arthritis, stiffness, and swelling of the knees.
Incorporating knee exercises into your daily routine will improve the strength of your knees. Knee strengthening exercises are a great non-invasive way to recover from arthritis and knee pain.
Here are a few knee exercises that target knee muscles for more flexible and stronger knees. Before you start you can begin by walking in place for 10-minutes to warm up. Here are five exercises to help you get started.
1. The Seated Knee Extension
The seated knee extension targets quadriceps, which are the muscles that help you straighten your knees. Working your quadriceps prevents or eliminates pain from your kneecaps. 
- Sit on a bench or chair with your shoulders back and down
- Place your feet on the floor and hands on your thighs
- Lift your left leg slowly to the level of your hips
- Hold for five seconds
- Place the foot back on the floor without locking your knees
- Perform this ten times for each leg.
2. The Standing Knee Flexion
This exercise strengthens your hamstrings, which are the muscles at the back of your thighs. It also boosts flexibility and knee balance. 
- Stand behind the back of a chair or bench
- Rest your arms on the chair or bench for balance
- In a 1-2-3 count, bend your leg as you can comfortably manage
Keep the supporting knee slightly bent as you lift the working leg
- Hold for approximately 5 seconds
- Return to the starting position in a 1-2-3 count
- Rest for 30 seconds and repeat the movement for each leg
3. Heel and Calf Raises
This exercise is a simple exercise that strengthens your calf and knees and boosts your knees’ support and stability.
- Stand with your feet flat on the floor in front of a wall for support
- Spread your legs shoulder-width apart
- Raise both heels off the floor and stand on your toes
- Hold for 6 seconds
- Lower your feet back to the floor
- Repeat ten times
With time, you can raise one foot at a time. Remember to keep your back straight, and do not lock your knees.
4. Single-Leg Dip
A single leg dip exercises the hamstrings and quadriceps for balance, knee strength, and joint stability.
- Stand between two chairs placed on the sides of your body with their backs next to your arms
- Place your hands on the backs of the chairs

- Lift your left leg slightly from the ground
- Slowly bend down, with your supporting knee forming a 90-degree angle
- Hold for 5 seconds
- Return to position
- Repeat with your right leg
Keep your back straight, and do not lean back while doing the exercise.
5. Wall Squats
Wall squats are great for your knees, as they build strength and stability in muscles and tissue supporting the knee joints.
- Stand facing 2 feet away from the wall
- Place your legs shoulder length apart
- Move your back down the wall, bending your knees to a 65% angle as if you are sitting on a chair
- Hold for 20 seconds
- Slowly get back to the standing position
- Repeat
Perform the exercise slowly, and don’t let your knees bend further than your toes.
When to Consider Physical Therapy
If you have been experiencing chronic knee pain or had knee surgery, consider a short-term rehabilitation facility to support your healing process.
At Church Home LifeSpring, we are committed to providing beneficial physical therapy to our patients. For information contact us to schedule an appointment.